The Achilles is the thickest tendon in your body, connecting your calf muscles to your heel bone. It helps to drive you forward as you run, walk and jump, therefore tolerating the highest loads in the body. Almost all the force created when pushing yourself forward travels through the Achilles tendon. This force can be between three to five times your bodyweight during running, jumping, hopping and skipping.
If you are unfortunate enough to injure your Achilles heel you may have something called Achilles tendonitis / tendinopathy.
What is Achilles tendonitis?
Achilles tendonitis or Achilles tendinopathy is the overuse of your Achilles tendon which results in injury. You will notice that when injured, the Achilles loses some of its ‘springy’ properties and becomes more supple. A thickened, slightly swollen lump in your tendon appears when you have a tendinopathy. This is caused by changes in the shape of the cells and collagen fibres that make up the tendon in response to the injury. This does not make the tendon weak, but it does make it difficult for it to tolerate increased loads.

What causes Achilles tendonitis?
There are certain risk factors that may cause someone to develop Achilles tendinopathy, most of which relate to changes in load through the tendon rather than to a person’s biomechanics. The tendon is worked too hard, so it develops an injury. It appears to be more common in men than women and tends to occur more often in one’s 30s or 40s. Some people also have a genetic predisposition to developing tendon pain.
Other risk factors include:
- Increasing training intensity – putting in an unusually hard training session or changing your training terrain (flat to hills) or volume can overload the Achilles. Also, not giving the tendon enough time to recover between hard training sessions, for example, speed or track sessions, hill running or plyometric exercises.
- Returning to training after a period of inactivity – going straight back into your training is also a big no. You need to ease your way into it again.
- Changes in training surface or footwear – wearing flatter trainers or switching to running more on the front of your feet will cause the Achilles to work harder than normal and may cause injury if you don’t introduce it slowly.
- Asymmetry in the biomechanics of the lower limb or lower back injuries can affect how you use the muscles in other parts of the body, which may play a role in you developing Achilles tendinitis/tendinopathy.
How do you know you’ve got Achilles tendonitis / tendinopathy?
Initially, athletes usually notice Achilles pain towards the end of a training session or a few hours after a run or high intensity activity.
Waking up with a painful tendon that makes you hobble for most of the day is common, but typical characteristics of Achilles tendinopathy are the onset of morning stiffness, which usually resolves after several minutes. This is often worse on days after activity. Aching in the tendon when getting up after sitting for extended periods is also a common symptom.
What is the treatment for Achilles tendinopathy?
There are several treatments that may help. Initially, the following treatments are usually recommended. They are all considered as ‘conservative’ treatments, meaning they do not involve surgery.
Rest
Rest from sporting activities are vital. Stopping any high-impact activities like running is important. When the pain diminishes, you can gradually resume exercising as the pain allows. There is a chain of thought that total, prolonged rest may actually be worse for the injury.
Painkillers
Painkillers, like paracetamol, may help to relieve pain. Non-steroidal anti-inflammatories (NSAIDs), like ibuprofen, may help too but only for short periods, because they may possibly reduce the ability of the tendon to heal in the long term. Always check with your doctor or pharmacist before taking NSAIDs to see if they are suitable for you, as there can be some negative side effects in certain people.
Ice
Ice therapy may help to minimise swelling in the early stages of Achilles tendinopathy. An ice pack should be applied for 10-15 minutes 3 times per day. More than 15 minutes at a time may damage the skin. If you don’t have an ice pack, a bag of frozen peas is a great alternative, but always wrap the bag in a damp towel beforehand as you may end up with an ice burn on your skin. Gently press the ice pack on to the tendon.
Achilles tendon exercises
Certain exercises to help to stretch and strengthen your Achilles tendon may be of benefit. You should try to do these every day, as these exercises may help with pain control and stiffness. One of our practitioners will be able to assist you with these exercises. They will also be able to use other treatment modalities, such as ultrasound and massage to help relieve symptoms and promote healing of the tendon.
Orthotics
Our Podiatrist may suggest changing your footwear or putting special inserts in your shoes, such as inserts to lift your heel to reduce the loading on your Achilles. This may help to reduce pain and symptoms.
What happens if initial treatment fails?
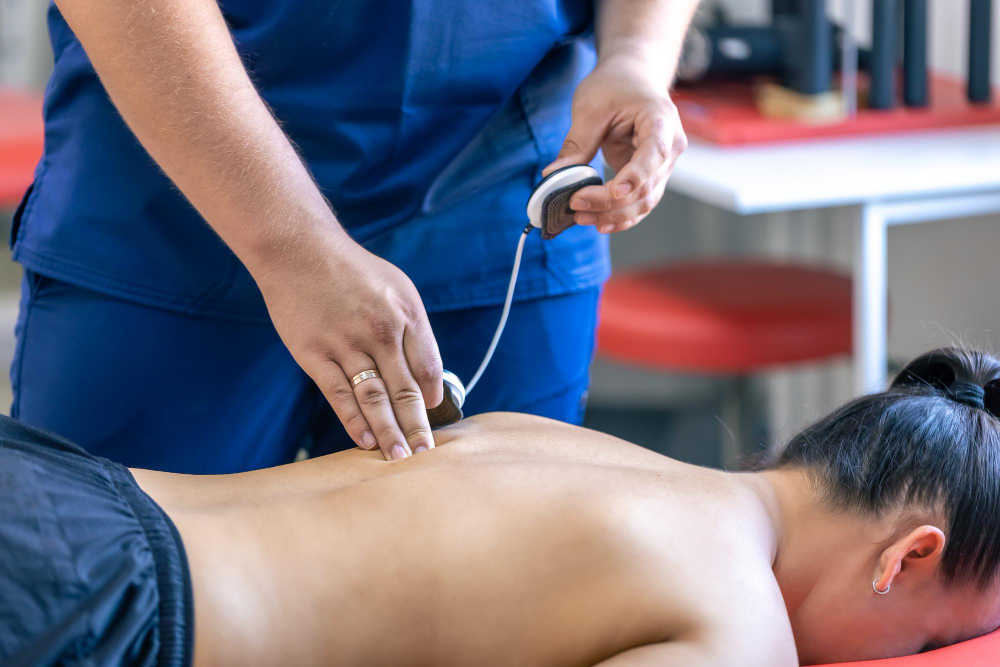
For the majority of people, symptoms of Achilles tendinopathy usually disappear within 3-6 months of starting conservative treatment. The outcome is usually better the sooner the issue is diagnosed and treatment started. If symptoms have not improved after a few months, there is an alternative, non-surgical treatment called Extracorporeal Shockwave Therapy. This is a non-invasive treatment performed with a hand-held device that creates high-energy sound waves (or pressure waves), transmitted to the injured tissue to provide pain relief.
Do I need surgery for Achilles tendinopathy?
Around 1 in 4 people who have continuing Achilles pain have surgery to treat the condition. Most people have a good result from surgery and their pain is relieved. Complications from surgery are rare but, if they do occur, can cause problems with wound healing.
If you would like to know more about the treatment we offer then please email us contact@carltoddclinics.com and one of our osteopaths or physiotherapists will be happy to help.
We are highly trained and have vast experience in the management and treatment of a wide range of sports injuries. We can help establish the cause of your injury and then create a treatment plan to help relieve your current symptoms. We can also advise on how to prevent future issues occurring.